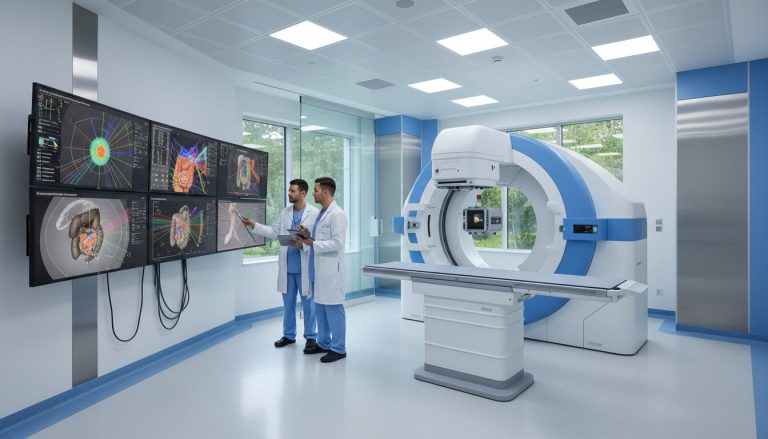
Hearing that you need radiation therapy can feel overwhelming. You likely have dozens of questions about how the process works, what it feels like, and how it will impact your daily routine. Before you receive a single dose of therapy, your medical team will take you through a crucial preliminary phase. This foundational step is known as Radiation Treatment Planning.
This mapping and preparation phase ensures that your therapy is as precise, safe, and effective as possible. When you know exactly what happens behind the scenes, you can approach your appointments with confidence and peace of mind. Let us explore the steps, the technology, and the people dedicated to your care.
This comprehensive guide walks you through every phase of radiation treatment planning. We break down the complex medical procedures into easy-to-understand steps, starting from your initial simulation to the rigorous quality assurance checks performed by your medical team.
You will discover actionable advice on avoiding common mistakes, practical pro tips to make your visits more comfortable, and proven strategies for managing potential side effects. By the end of this guide, you will have a clear, thorough understanding of your treatment roadmap, empowering you to take an active role in your healthcare journey.
Understanding Radiation Treatment Planning
Radiation Treatment Planning is a highly customized medical process designed to map out exactly how your radiation therapy will be delivered. Cancer cells are vulnerable to high-energy beams, but your healthy tissues need protection. The primary goal of this planning phase is to maximize the dose delivered to the tumor while minimizing the exposure to surrounding healthy organs.
Every patient’s anatomy is entirely unique. Two people with the exact same type of cancer will still require completely different treatment plans based on their body shape, the exact location of the tumor, and their overall health. This is why the planning phase is so meticulous.
During this time, a specialized team of experts works together on your behalf. Your radiation oncologist leads the charge, determining the total dose of radiation you need. They collaborate closely with a medical dosimetrist, who uses advanced computer software to design the beam arrangements. Finally, a medical physicist ensures the machines are perfectly calibrated to deliver the exact dose prescribed safely.
This collaborative effort forms the backbone of your treatment. Taking the time to build a flawless plan is just as critical as the treatment itself. When your team invests days into mapping your body, they are building a customized shield and targeted strategy specifically for you.
The Planning Process of Radiation Treatment
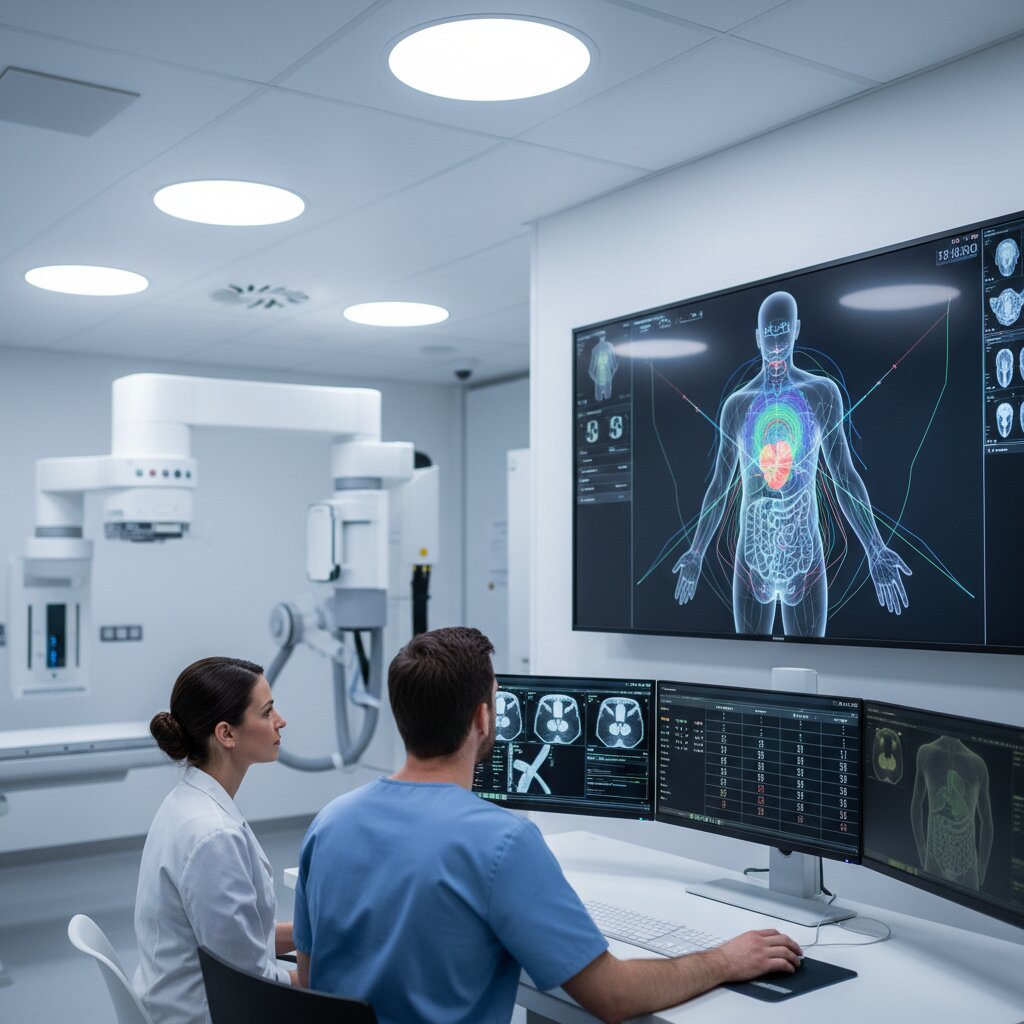
The journey of radiation treatment planning involves several distinct phases. You will only be present for the first part, while your medical team handles the rest behind the scenes.
CT Simulation
Your active role in the planning process begins with a session called simulation. A simulation is exactly what it sounds like: a dry run of your future treatments. You will not receive any radiation therapy during this visit. Instead, the team uses a CT scanner to create a three-dimensional map of your body.
When you arrive, your radiation therapists will help you onto the scanning table. Because precision is critical, you must remain perfectly still during your actual treatments. To help you do this, the team will create custom immobilization devices. If you are receiving treatment on your head or neck, this might be a warm, flexible mesh mask that molds to your face and hardens. For pelvic or chest treatments, you might lie in a custom body mold or vacuum cushion. These devices ensure you are in the exact same position every single day.
Once you are comfortable and immobilized, the CT scan begins. In some cases, you may be asked to swallow a contrast liquid or receive an IV contrast dye to help certain organs show up more clearly on the scan. You might also be coached on specific breathing techniques, such as holding your breath for a few seconds, to keep your internal organs from moving.
After the scan, the therapists will place tiny alignment marks on your skin. These are often small, permanent freckle-sized tattoos. These marks act as a target for the laser crosshairs in the treatment room, ensuring flawless alignment for every session.
Designing the Treatment Plan
Once you leave the simulation appointment, the behind-the-scenes work begins. The high-resolution images from your CT scan are sent to complex treatment planning computers.
First, your radiation oncologist carefully reviews the scans. They digitally outline the exact borders of the tumor, a process called contouring. Just as importantly, they outline the healthy organs nearby that must be protected. For example, if you are treating the left breast, the doctor will carefully outline the heart and lungs to ensure they receive minimal exposure.
Next, the medical dosimetrist takes over. Using specialized algorithms, they calculate the best angles and intensities for the radiation beams. They might use a technique called Intensity-Modulated Radiation Therapy (IMRT), which allows them to adjust the strength of the beam in millimeter increments. The dosimetrist runs multiple virtual scenarios, looking for the perfect balance between attacking the cancer and sparing healthy tissue.
This phase can take anywhere from a few days to two weeks. The team will not rush this process. They will tweak the digital model continuously until the plan meets the highest clinical standards.
Quality Assurance
Before you ever return for your first actual treatment, your personalized plan undergoes a rigorous quality assurance (QA) phase. The medical physicist runs your exact treatment plan on the linear accelerator—the machine that will deliver your radiation.
They use special phantoms (devices that mimic human tissue) to measure the Radiation Treatment Planning coming out of the machine. They verify that the dose the computer calculated is the exact dose the machine delivers. They also check the mechanical movements of the machine, ensuring the gantry rotates properly and the internal metal leaves shape the beam exactly as prescribed.
Only after the physicist, dosimetrist, and oncologist all sign off on the plan’s safety and accuracy will you be called in for your first treatment session.
Common Mistakes to Avoid of Treatment Planning

Navigating radiation treatment planning can be intimidating, and it is easy to make simple mistakes. Being aware of these common pitfalls can make your experience significantly smoother.
Ignoring Pre-Simulation Instructions
Depending on the area being treated, your team may give you specific instructions before your simulation. For example, patients treating prostate or pelvic cancers are often asked to arrive with a comfortably full bladder and an empty rectum. This pushes the intestines up and out of the Radiation Treatment Planning field. Failing to follow these prep instructions can delay your simulation or result in a less-than-optimal scan. Always ask for written instructions and follow them closely.
Washing Off Temporary Marks
While many clinics use tiny permanent tattoos, some still use temporary ink or tape to mark your skin during simulation. It can be incredibly tempting to scrub these off in the shower, especially if they smudge or feel sticky. Do not touch them. These marks are the exact coordinates for your treatment. If you wash them off, you may have to repeat the entire simulation process. If you notice a mark fading, tell your therapists so they can darken it.
Staying Silent About Discomfort
During the simulation, you will be placed in a specific position that you will need to hold for 15 to 30 minutes every day during treatment. If the armrest pinches your shoulder, or the knee cushion hurts your back, you must speak up immediately. If you try to “tough it out” during the simulation, you will be stuck in that uncomfortable position for weeks. Your therapists can easily adjust the immobilization devices to make you comfortable, but they can only do so if you tell them.
Pro Tips for Patients
Taking a proactive approach to your treatment planning can drastically reduce anxiety. Here are several expert insights to help you navigate this phase.
Wear Practical Clothing
On the day of your simulation and subsequent treatments, dress for comfort and convenience. Wear loose-fitting clothes that are easy to take off and put on. Avoid tight collars, restrictive belts, or complicated buttons. If you are having a body mold made, you may need to wear a hospital gown. Slip-on shoes are a great choice, as you will be taking them off to lie on the treatment table.
Ask About Music
Lying still on a hard table while a large machine circles you can feel isolating. Many modern Radiation Treatment Planning oncology departments have audio systems integrated into the treatment rooms. Ask your therapists if you can listen to a specific genre of music, a favorite artist, or even a podcast during your simulation and daily setups. Focusing on the audio can make the time pass much faster and keep you relaxed.
Bring a Support Person
There is a lot of information to absorb during the consultation and simulation phase. Bring a trusted friend or family member with you. They can act as a second set of ears, write down important instructions, and provide emotional support while you are in the waiting room.
Prepare a Medical History Summary
Your radiation oncologist will need a comprehensive view of your health. Bring a printed list of all medications you currently take, including over-the-counter supplements and vitamins. Also, be prepared to discuss any past surgeries, especially if you have ever had Radiation Treatment Planning therapy before or if you have any implanted medical devices like a pacemaker or artificial joints.
Managing Side Effects of Medical Treatment

It is important to note that you will not experience any side effects from the CT simulation or the Radiation Treatment Planning treatment planning process itself. The simulation uses standard diagnostic X-rays, which do not cause immediate physical symptoms.
However, as you transition from planning into your actual daily treatments, side effects may begin to appear. Being prepared for these can help you manage them effectively.
Skin Irritation
The most common side effect is skin irritation in the exact area being treated. After a few weeks of treatment, your skin may look and feel like it has a sunburn. It might become red, dry, itchy, or prone to peeling. To manage this, avoid using harsh soaps or applying extreme heat or cold (like heating pads or ice packs) to the area. Your care team will recommend specific, fragrance-free lotions. Apply them generously, but wait until after your daily treatment session to put them on.
Fatigue
Radiation therapy requires your body to use massive amounts of energy to repair healthy cells that are incidentally affected. Because of this, cumulative fatigue is highly common. This is not the type of tiredness that goes away with a single nap. Listen to your body. Adjust your daily schedule to allow for rest periods, prioritize a nutrient-dense diet, and stay highly hydrated. Light, gentle exercise, such as a short daily walk, can actually help boost your energy levels and combat this fatigue.
Area-Specific Side Effects
Other side effects depend entirely on where your customized plan directs the Radiation Treatment Planning. If you are receiving treatment to the head and neck, you might experience a dry mouth, changes in taste, or difficulty swallowing. If the treatment targets your pelvis, you may notice changes in urination or bowel habits. Your doctor will discuss these specific localized risks with you when they present your finalized treatment plan.
Conclusion
Understanding the meticulous nature of Radiation Treatment Planning treatment planning can transform a daunting medical procedure into a structured, manageable journey. From the precision of the CT simulation to the rigorous safety checks performed by your medical team, every step is designed specifically to protect your health and target your illness. Remember to follow your pre-appointment instructions, communicate openly with your therapists, and prepare your body for the road ahead. If you are ready to take the next step in your care, reach out to your oncology team today to review your personalized treatment timeline and get your questions answered.
Frequently Asked Questions
1. What exactly is a CT simulation in radiation treatment planning?
A CT simulation is the very first physical step in mapping out your therapy. You will lie on a scanner table in the exact position you will use for your daily treatments. The scanner takes detailed 3D images of your internal anatomy, which your medical team uses to design a highly accurate, customized Radiation Treatment Planning delivery plan. No actual radiation therapy is given during this visit.
2. How long does the radiation treatment planning process take?
The simulation appointment itself usually takes about 45 to 60 minutes. However, the background work—where the dosimetrist and physicist calculate angles, doses, and run quality assurance tests—can take anywhere from a few days to two weeks. Your doctor will give you a specific timeline for when your actual treatments will begin.
3. Do the permanent tattoo marks hurt?
The alignment marks are incredibly small, usually the size of a freckle or a pinhead. The process of getting them feels like a quick pinprick or a tiny scratch. It takes only a second per mark, and the discomfort is minimal and fades almost instantly. These marks are crucial for aligning the lasers to ensure flawless daily setups.
4. Can I wash my skin after the simulation?
If your team uses permanent tattoos, you can shower and wash normally immediately after the appointment. However, if they use temporary ink or tape to mark your skin, you must be very careful not to scrub or wash them off. Always ask your Radiation Treatment Planning therapists for specific bathing instructions before leaving your simulation.
5. Why do I need to hold my breath during the scan?
For certain types of cancer, particularly left-sided breast cancer or lung cancer, you may be asked to hold your breath for short bursts. This technique, called Deep Inspiration Breath Hold, inflates your lungs and pushes your heart away from the chest wall. This creates a larger buffer zone, minimizing the amount of radiation that reaches your heart tissue.
6. Will I be radioactive after my simulation or daily treatments?
No. The vast majority of radiation therapy is delivered via external beam radiation. The energy passes through your body to target the tumor, much like a standard X-ray. You will not be radioactive, and it is completely safe to be around your family, friends, children, and pets immediately after you leave the clinic.
7. What happens if I move during the simulation?
Precision is the most important factor in Radiation Treatment Planning treatment planning. If you sneeze, cough, or shift your body significantly during the CT scan, the images will be blurry or inaccurate. The therapists will likely need to stop the scanner, reposition you, and start the scan over. This is why the custom immobilization devices are so important.
8. Who is responsible for designing my treatment plan?
Designing your plan is a collaborative effort. Your radiation oncologist prescribes the total dose and outlines the target areas. A medical dosimetrist uses advanced software to calculate the beam paths and angles. A medical physicist oversees the technical safety, ensuring the computer plan can be perfectly executed by the linear accelerator.
9. Can I take my normal medications on the day of my simulation?
In most cases, yes, you should take your regular medications as prescribed. However, if your simulation requires an empty stomach or a specific bowel preparation, you may need to adjust when you take oral medications. Always provide your doctor with a full list of your prescriptions and follow their specific guidance for simulation day.
10. What should I do if my immobilization mask makes me feel claustrophobic?
It is very common to feel anxious when wearing a tight-fitting mesh mask over your face and neck. Inform your therapists immediately if you feel panicked. They can often cut larger eye or mouth holes in the mask to help you feel less restricted. Practicing deep, slow breathing and listening to calming music can also significantly reduce claustrophobia during the scan.