Receiving infusion therapy can be a defining moment for anyone battling malignancy. In today’s digital landscape, understanding each aspect of infusion for cancer patients plays a vital role in fostering confidence and alleviating anxiety. Currently, more specialized medications are delivered directly into the bloodstream, bypassing the digestive tract to enhance efficacy. In this year (2026), clinicians continue to refine infusion methods, ensuring a safer and more tailored experience for those undergoing treatment. This comprehensive guide will explore the fundamentals of infusion protocols, outline what to anticipate during each visit, and offer practical strategies for managing side effects. By the end, you will have an actionable plan designed to help you navigate your healthcare journey with clarity and empowerment.
Understanding Infusion Therapy in Modern Oncology
Infusion therapy offers a direct pathway to introduce potent medications into the bloodstream, an approach that is particularly valuable when treating complex diseases such as cancer. For infusion for cancer patients, the process typically involves accessing a vein through a temporary intravenous catheter, a peripherally inserted central catheter (PICC), or an implanted port. These delivery systems allow healthcare teams to administer precise doses over controlled timeframes, improving absorption and reducing variability that can occur with oral administration. Today’s infusion pumps deliver medication at a steady rate, minimizing fluctuations in concentration and ensuring that the therapeutic effect remains within an optimal window. Modern oncologists choose infusion as a method because it bypasses the digestive tract, which can degrade or delay some drugs.
Another key advantage of infusion lies in its versatility. Clinicians can adjust infusion rates based on real-time monitoring of vital signs and patient tolerance. In cases of severe nausea or hypersensitivity reactions, doses can be paused or slowed to protect the patient without compromising the overall treatment plan. Additionally, combination therapies—such as pairing cytotoxic agents with immunotherapy—are often administered sequentially during the same appointment. This integrated approach allows infusion for cancer patients to gain the benefits of multiple mechanisms of action within a single session. Infusion also supports dose-dense regimens, where closer scheduling enhances efficacy against rapidly dividing cells.
From a logistical standpoint, outpatient infusion centers have become increasingly sophisticated. Many are outfitted with reclining chairs, personal entertainment systems, privacy curtains, and access to snack stations. Nurse specialists trained in oncology monitor infusion for cancer patients, checking blood pressure, temperature, and infusion site integrity at regular intervals. Communication channels between nursing staff and pharmacy teams are robust, ensuring that any necessary dose adjustments or premedications—such as antiemetics or antihistamines—are delivered promptly. This level of coordination improves safety and contributes to a more comfortable experience for the patient.
In today’s digital landscape, electronic health records (EHR) track infusion schedules, adverse events, and laboratory values in real time. Tools like computerized physician order entry (CPOE) reduce the risk of dosing errors, while barcode scanning systems confirm patient identity and medication accuracy. According to the National Cancer Institute, such technological integrations have significantly decreased the incidence of infusion-related complications in recent years. As research continues to evolve, infusion techniques remain at the forefront of oncology treatment, demonstrating that targeted delivery is a cornerstone in supporting positive outcomes for those receiving care.
The decision to recommend infusion for cancer patients takes into account factors such as cancer type, stage, genomic markers, and the patient’s overall health status. Tumors with specific molecular targets—identified through next-generation sequencing—often benefit from targeted therapies that require steady blood levels achieved via infusion. Immunotherapies, including checkpoint inhibitors, rely on a sustained presence in circulation to modulate the immune response. Even supportive treatments, such as hydration solutions, antibiotics or growth factors, are administered by infusion to maintain blood counts, prevent infection, and manage treatment-induced side effects. Collaborating with a multidisciplinary team ensures that infusion protocols align with personalized care plans, reflecting a holistic approach to patient well-being.
Exploring Diverse Infusion Regimens in Cancer Care
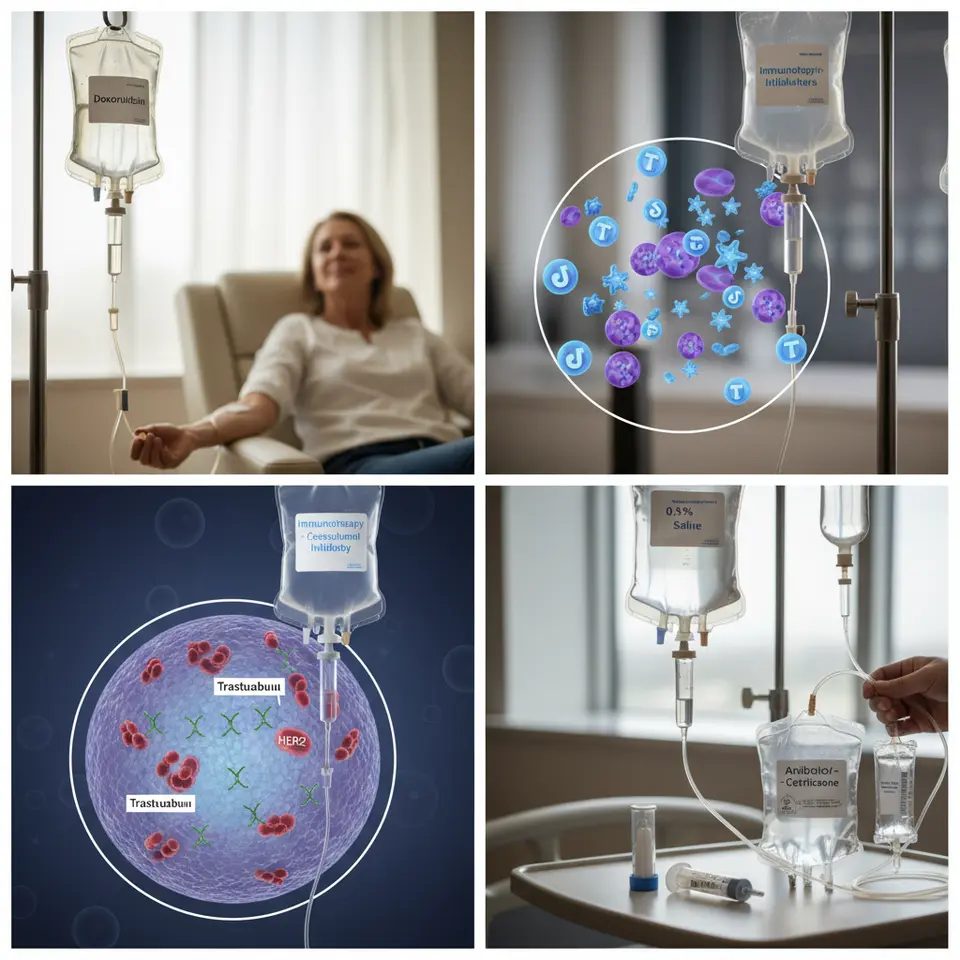
Chemotherapy remains a cornerstone in cancer treatment, using cytotoxic agents that target rapidly dividing cells. When administered by infusion, these drugs achieve high plasma concentrations without the need for multiple daily pills. Agents such as doxorubicin, cisplatin and paclitaxel are commonly infused according to calculated body surface area and weight-based protocols. For infusion for cancer patients, chemotherapy schedules are often divided into cycles. A typical regimen may involve an infusion day followed by rest periods, allowing healthy tissue to recover. Advances in pump technology enable programmable delivery, meaning some regimens extend over several days via portable ambulatory pumps, granting patients greater mobility and convenience while maintaining therapeutic effectiveness.
Immunotherapy harnesses the body’s immune defenses to recognize and eliminate malignant cells. Checkpoint inhibitors, such as pembrolizumab and nivolumab, are delivered intravenously at set intervals—often every two to three weeks. These infusions release the brake on immune cells, empowering them to detect and destroy cancer cells. Other immunotherapies include adoptive cell transfer and CAR T-cell therapy, which also rely on infusion techniques to reintroduce engineered immune cells into the patient’s circulation. According to the Centers for Disease Control and Prevention, infusion-based immunotherapies have significantly improved survival rates for various cancer types in recent years.
Targeted therapies focus on molecular abnormalities unique to tumor cells. Small molecule inhibitors, such as imatinib or erlotinib, are typically oral, but some monoclonal antibodies targeting growth factor receptors—like trastuzumab for HER2-positive breast cancer—require infusion. These biologics bind to specific proteins on cancer cells, blocking growth signals and marking cells for destruction. Infusion for cancer patients with targeted agents often involves a loading dose followed by maintenance infusions at regular intervals, enabling sustained blockade of oncogenic pathways.
Supportive infusions play a crucial role in managing collateral effects of primary treatments. Hydration solutions help flush toxins produced during cytotoxic therapy, reducing the risk of kidney damage. Infusions of colony-stimulating factors, such as granulocyte colony-stimulating factor (G-CSF), support white blood cell production, lowering infection risk. Pain management may involve opioid infusions or intravenous analgesics for patients with severe discomfort. Antibiotics delivered by infusion address infections that can arise due to immunosuppression. Bone-strengthening agents, including bisphosphonates or denosumab, are infused to prevent tumor-related bone breakdown and reduce fracture risk.
Designing an infusion regimen requires close collaboration between oncologists, nurses, and pharmacists. Factors such as renal function, liver enzymes, and prior treatment history influence drug selection and dose adjustments. Personalized infusion schedules may also incorporate pharmacokinetic monitoring to tailor dosages based on blood levels and clearance rates. This individualized approach ensures that each patient receives an optimal balance of efficacy and tolerability. In today’s digital landscape, treatment teams utilize EHR-integrated decision support systems to compare standardized protocols with patient-specific data, reducing errors and enhancing the safety of infusion for cancer patients.
Preparing for Your Infusion Session: Expectations and Logistics
Before attending an infusion appointment, you will likely receive specific instructions from your oncology team regarding pre-treatment steps. This may include fasting guidelines, reminders to hydrate, and a list of medications to take before arrival—often anti-nausea drugs or steroids aimed at reducing the risk of adverse reactions. On the day of infusion, patients typically check in at an outpatient infusion center or a designated hospital unit. Today, many facilities offer online check-in options through patient portals, streamlining the admission process and minimizing waiting times for infusion for cancer patients.
Upon arrival, a nurse will review your current health status, confirming recent laboratory results, vital signs, and any new symptoms. Access to your vein is then established. Depending on the expected number of treatment cycles, this might be through:
- PICC line: A flexible catheter inserted into a large vein in the arm.
- Implanted port: A small reservoir placed under the skin, accessed with a special needle.
- Peripheral IV: A temporary catheter placed in a vein on the hand or forearm.
Each device has advantages; implanted ports, for example, reduce the need for repeat needle sticks and are less prone to dislodgement. Once the access is secured, your healthcare provider will connect you to an infusion pump calibrated to deliver the prescribed dose over a predetermined period. Infusion durations vary widely: a simple hydration infusion may take 30 minutes, while complex chemotherapy combinations can extend to several hours or even multi-day regimens.
Throughout the session, nurses monitor key parameters such as blood pressure, heart rate, temperature, and oxygen saturation at regular intervals. They also watch for signs of infusion-related complications—ranging from mild symptoms like chills and itching to more serious reactions such as difficulty breathing or rapid swelling. Good communication is essential; patients are encouraged to report any discomfort immediately. Infusion centers now often integrate real-time electronic documentation systems to track these observations and share information with the broader care team instantly, enhancing both safety and continuity of care.
To make lengthy sessions more comfortable, many infusion facilities provide reclining chairs, personal entertainment screens, and Wi-Fi access. Some even feature quiet rooms or private bays. Patients commonly bring books, headphones, snacks, or a travel mug with their favorite beverage to pass the time. Support persons are usually welcome to accompany the patient, offering emotional reassurance. In this year (2026), remote monitoring devices and mobile applications can send updates to your care team, allowing them to intervene quickly if vital signs stray beyond safe limits. Being well-informed about each step helps infusion for cancer patients feel more predictable, reducing anxiety and supporting a smoother treatment experience.
Managing Side Effects and Enhancing Recovery
While infusion therapy is a powerful tool against cancer, patients may experience a range of side effects during and after treatment. Common immediate reactions include flushing, chills or fever, which often respond well to slowing or temporarily pausing the infusion. More persistent issues such as fatigue, nausea, and cognitive changes—sometimes referred to as “chemo brain”—can develop hours to days after your session. Proactively planning for these effects can significantly improve quality of life for infusion for cancer patients.
Nutritional support plays a major role in managing treatment-induced side effects. Eating small, frequent meals rich in protein and healthy carbohydrates can help counteract nausea and maintain energy levels. According to guidelines from the National Cancer Institute, incorporating ginger, mint teas, or cold foods like smoothies may soothe an upset stomach. If taste alterations become problematic, experimenting with different textures—crisp vegetables or flavored broths—can make mealtime more tolerable. It is also important to stay hydrated; oxygen-rich solutions with electrolytes may be recommended if vomiting or diarrhea occurs.
Fatigue is another prevalent concern. Listening to your body and scheduling rest periods is essential. Short naps, light stretching or yoga routines, and gentle activities such as walking can help maintain muscle tone and boost mood. Some infusion for cancer patients benefit from keeping a daily journal to track energy levels, identify patterns, and communicate concerns to the care team. Occupational therapists can provide personalized exercises to improve cognitive functioning and support day-to-day tasks when mental fog sets in.
Mucosal issues—such as mouth sores—may arise during certain infusions, particularly those involving 5-fluorouracil or methotrexate. Prevention strategies include maintaining meticulous oral hygiene with soft-bristled toothbrushes, using prescribed mouth rinses, and avoiding acidic or spicy foods. For hand-foot syndrome—a condition marked by redness, swelling and pain on the palms and soles—applying thick moisturizing creams and wearing loose-fitting shoes can offer relief. If chronic neuropathy develops, medications like gabapentin or topical lidocaine may be prescribed to manage discomfort.
Psychosocial support is equally important this year (2026). Counseling, support groups, and digital communities provide a platform to share experiences and coping strategies. Some infusion centers now integrate on-site counseling services or refer patients to accredited support organizations. Engaging with others who are navigating similar challenges helps reduce isolation and fosters resilience. Effective communication with your oncology team—reporting side effects early and adjusting supportive medications—ensures that infusion for cancer patients remains not only effective but also as comfortable as possible.
Given that infusion treatments can impact blood cell counts, patients must monitor for signs of infection, such as persistent cough or unusual bruising. Routine blood tests before each session measure white blood cell levels, platelets, and other indicators. If neutropenia—low white blood cell count—occurs, physicians may delay treatment or administer growth factor injections. Strict adherence to hand hygiene, avoiding crowded places during peak cold season, and staying up to date on recommended vaccinations are proactive measures that infusion for cancer patients can take to safeguard overall health.
Optimizing Nutrition, Hydration, and Lifestyle During Treatment
For infusion for cancer patients, maintaining balanced nutrition and proper hydration is as crucial as the medications themselves. Today, oncology dietitians emphasize personalized meal plans that provide essential macro- and micronutrients to support healing and energy. Prior to each session, drinking at least 8 to 10 cups of water or clear fluids helps ensure that kidneys can efficiently eliminate byproducts of chemotherapy. Electrolyte-infused beverages may be recommended if you experience diarrhea or vomiting, helping to restore sodium, potassium and magnesium levels.
Choosing the right foods can also minimize treatment complications. A diet rich in lean proteins—such as eggs, fish, poultry, beans and lentils—supports muscle repair and immune function. Antioxidant-rich fruits and vegetables, including berries, leafy greens and cruciferous vegetables, may help neutralize free radicals generated during infusion inflictions. However, infusion for cancer patients with compromised immunity should avoid raw or undercooked items to reduce infection risk. The Centers for Disease Control and Prevention recommends thoroughly washing produce, cooking meats to safe internal temperatures, and avoiding unpasteurized dairy products or juices.
Small, frequent meals can counteract appetite changes and nausea. Snacking between meals with nutrient-dense options—nuts, Greek yogurt, hummus with whole-grain crackers—can sustain calorie intake. Some patients find benefit in keeping a “go bag” stocked with portable snacks, such as trail mix or protein bars, for use during long infusion sessions. Incorporating healthy fats from sources like avocados, olive oil and fatty fish also contributes to overall caloric and nutrient needs.
Beyond diet and fluids, adjusting daily routines can improve treatment tolerance. Light physical activity, including walking, gentle yoga or tai chi, supports circulation, mood and muscle strength. Adequate sleep—aiming for 7 to 9 hours each night—helps the body repair and cope with therapy-induced stress. Infusion for cancer patients may also benefit from relaxation techniques such as deep breathing exercises, meditation or guided imagery to reduce anxiety and enhance emotional well-being.
Sun protection and skincare warrant attention, especially when skin reactions or sensitivity occur due to certain infusions. Applying broad-spectrum sunscreen, wearing protective clothing, and using fragrance-free moisturizers can prevent dryness and irritation. Avoiding herbal supplements without prior approval is essential; some botanicals may interfere with treatment metabolism or increase bleeding risk. Always discuss any vitamins, probiotics or alternative remedies with your oncology provider before adding them to your regimen.
In today’s interconnected healthcare environment, digital tools can further support infusion for cancer patients. Mobile apps designed to track hydration, medication schedules, symptom diaries and appointment reminders empower patients to stay organized and engaged in their care. Regular follow-ups, either in person or via telehealth, ensure that any emerging concerns receive timely attention. By adopting a holistic lifestyle approach—combining nutrition, fluid management, physical activity and mental health strategies—you can reinforce the effectiveness of infusion therapy and maintain the best possible quality of life.
Frequently Asked Questions
- What is infusion therapy and why is it used in cancer treatment?
Infusion therapy delivers medications directly into the bloodstream for faster, more reliable absorption and precise dosing, which is especially important for chemotherapy, immunotherapy, and supportive treatments. - How long does an infusion session typically last?
Infusion durations vary: simple hydration may take 30 minutes, standard chemotherapy infusions often run 1–4 hours, and complex or multi-day regimens use ambulatory pumps for extended delivery. - What should I do to prepare for my infusion appointment?
Follow your oncology team’s instructions on fasting, hydration, and premedications. Bring identification, a list of current medications, snacks, entertainment, and any comfort items for a smoother visit. - How can I manage side effects at home between sessions?
Stay well-nourished with small, frequent meals; keep hydrated; rest appropriately; maintain good oral hygiene; and report any concerning symptoms to your care team promptly. - Are there risks with implanted ports or PICC lines?
While these devices reduce needle sticks and improve ease of access, they carry risks like infection or thrombosis. Proper site care and prompt reporting of redness, swelling, or pain are essential.
Conclusion
Infusion for cancer patients represents a dynamic convergence of medical science, patient-centered care and technological innovation. By delivering medications directly into the bloodstream, infusion therapies offer improved precision and reliability, supporting a wide range of treatments from chemotherapy to immunotherapy and targeted biologics. In this year (2026), infusion protocols continue to evolve, benefiting from data-driven adjustments and digital monitoring systems that enhance safety and effectiveness.
Successfully navigating infusion care involves understanding each step of the process, preparing for potential side effects and embracing supportive strategies such as optimal nutrition, hydration and lifestyle modifications. Collaboration with a multidisciplinary healthcare team—comprising oncologists, nurses, pharmacists and dietitians—ensures that every infusion aligns with your personalized treatment goals. Remember to ask questions, report symptoms promptly and leverage community resources, including reputable organizations like the National Cancer Institute and the Centers for Disease Control and Prevention, which offer evidence-based guidance.
By staying informed, proactive and connected to your care network, you can maximize the benefits of infusion therapy while preserving your well-being. Empowered with knowledge and supported by skilled professionals, each infusion visit becomes an opportunity to advance your journey toward recovery. Embrace these strategies and trust in the collective expertise guiding you every step of the way. Ultimately, your resilience combined with these tools will help you face challenges with strength and hope as you progress through treatment.


