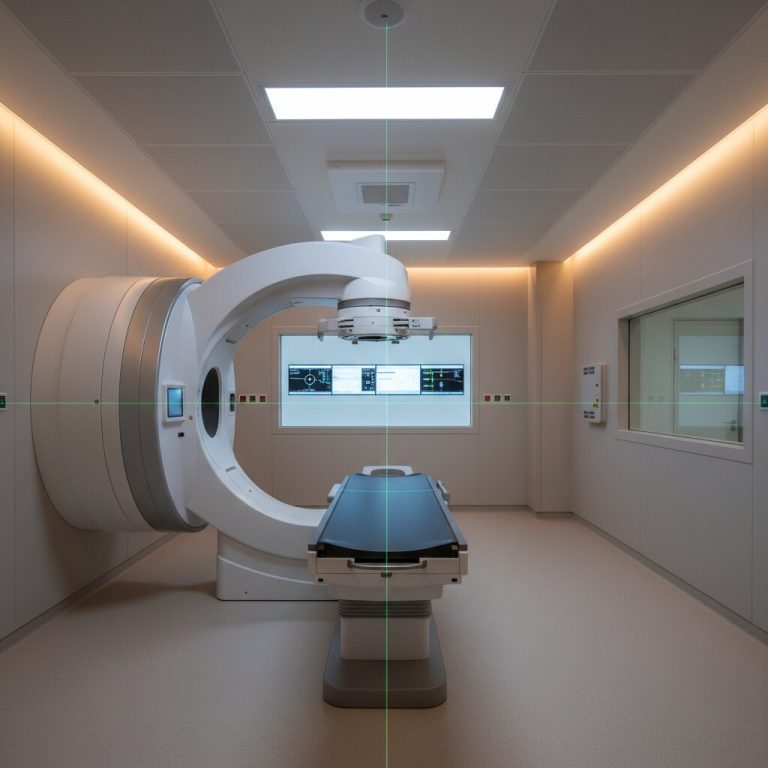
Facing cancer treatment feels overwhelming, but visualizing the process brings comfort. Reviewing photos of radiation therapy helps you prepare mentally. We will explore exactly what happens in the treatment room so you can face your upcoming sessions with absolute confidence.
This comprehensive guide demystifies the entire radiation treatment process. We explore preparation steps, daily session expectations, and side effect management. By understanding the machinery and environment through photos of radiation therapy, you reduce anxiety. You will learn actionable expert tips, common mistakes to avoid, and strategies for a smoother recovery.
Why Photos of Radiation Therapy Matter
Stepping into a cancer treatment center for the first time brings a flood of emotions. The environment looks clinical, the machines appear massive, and the fear of the unknown takes over. This is exactly where photos of radiation therapy provide immense value. By looking at images of the treatment rooms, the linear accelerators, and the immobilization devices beforehand, you remove the shock factor.
Visualizing the Unknown
Humans process visual information rapidly. When you view photos of radiation therapy, you familiarize your brain with the clinical environment. You see the table where you will lie down. You see the large machine that will move around you. This visual preparation bridges the gap between terrifying medical jargon and reality. Knowing what the equipment looks like empowers you to walk into your first session with a sense of control.
Understanding Radiation Therapy: An Overview
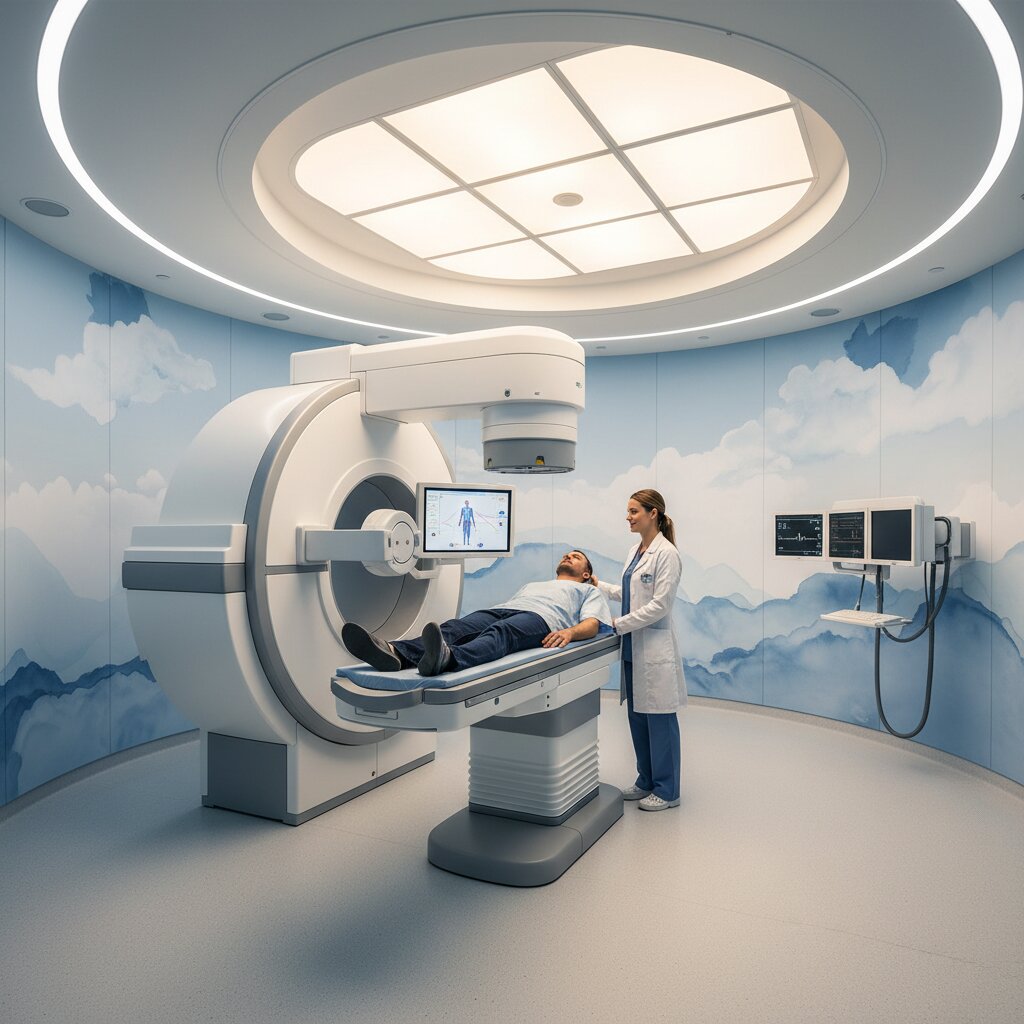
Before diving into the exact steps of your daily visits, you must understand what radiation therapy actually does. Medical professionals use high doses of radiation to destroy cancer cells and shrink tumors.
What is Radiation Therapy?
Radiation therapy, also known as radiotherapy, uses intense beams of energy to kill cancer cells. Most treatments utilize X-rays, though some use protons or other types of energy. The radiation damages the DNA inside the cancer cells. When the DNA suffers enough damage, the cells stop dividing and die. The body then naturally breaks down and eliminates these dead cells.
If you look at diagrams or photos of radiation therapy mechanisms, you will notice that the beams target a very specific area. Modern technology allows oncologists to focus the energy precisely on the tumor while sparing the surrounding healthy tissue.
The Goals of Treatment
Doctors use radiation therapy for several distinct reasons. Sometimes, it serves as the primary treatment to cure the cancer completely. Other times, doctors use it before surgery to shrink a tumor (neoadjuvant therapy) or after surgery to stop remaining cancer cells from growing (adjuvant therapy). In advanced cases, radiation helps relieve symptoms and improve quality of life, which doctors call palliative care.
Step-by-Step Guide: Before Treatment Begins
Your journey does not start with the radiation machine. A significant amount of planning happens behind the scenes to ensure your safety and treatment efficacy.
The Consultation
Your first step involves meeting with a radiation oncologist. This specialist reviews your medical records, pathology reports, and imaging scans. Together, you will discuss the potential benefits and risks of the treatment. Your doctor will explain how many sessions you need and what specific type of radiation suits your condition.
The Simulation Process
Simulation represents the most crucial planning phase. During this appointment, the radiation therapy team maps out your exact treatment plan. You will lie on a table identical to the one used for actual treatment.
If you search for simulation photos of radiation therapy, you will see patients wearing special masks or lying in custom body molds. These immobilization devices ensure you remain in the exact same position for every single treatment session.
The team will also make small marks on your skin. Sometimes they use a temporary marker, and sometimes they use tiny permanent tattoos the size of a freckle. These marks act as a map for the radiation therapists to align the machine perfectly each time. During this visit, the team will also take CT or MRI scans while you rest in your treatment position.
Step-by-Step Guide: During Treatment
Once the planning phase ends, your actual treatment sessions begin. Most patients receive external beam radiation therapy five days a week for several weeks.
Entering the Treatment Room
When you arrive for your daily session, a radiation therapist will guide you into the treatment room. The room features a large machine called a linear accelerator. If you have studied photos of radiation therapy, this machine will look very familiar. It consists of a long treatment table and a massive, rotating arm that delivers the energy beams.
Positioning and Immobilization
The therapist will help you onto the table. They will use the custom molds, cushions, or masks created during your simulation to hold your body in the correct posture. You must remain completely still during the treatment. Being comfortable is vital, so always inform your therapist if a cushion feels wrong or a mask pinches your skin.
The Machine in Action
Once the therapist positions you perfectly using the marks on your skin and laser lights on the walls, they will leave the room. You will be alone, but the therapist watches you on a video monitor and can hear you through an intercom.
The linear accelerator will begin to move around you. It makes buzzing and clicking sounds, which is entirely normal. You will not see, smell, or feel the radiation. The entire process resembles getting a standard X-ray.
The actual delivery of the radiation takes only a few minutes. Most of your 15-to-30-minute appointment involves positioning your body accurately. Many facilities allow you to listen to music during this time to help you relax.
Step-by-Step Guide: After Treatment
Because external beam radiation operates on an outpatient basis, you will go home immediately after your session. You do not become radioactive, and you pose no danger to your family members, children, or pets.
Immediate Aftermath
Right after a session, you can usually resume your normal daily activities. Some people drive themselves to and from their appointments and even go to work afterward. However, as the weeks progress, the cumulative effect of the treatments may start to alter your routine.
Follow-Up Care
You will meet with your radiation oncologist at least once a week during your treatment course. They will check your progress, examine your skin, and discuss any side effects you experience. Open communication during these visits is crucial. Do not hide your symptoms; your medical team possesses many tools to help you manage discomfort.
Common Side Effects and How to Manage Them
Radiation targets cancer cells, but it also affects healthy cells in the treatment area. This causes side effects. Fortunately, healthy cells repair themselves much better than cancer cells do.
Fatigue
Fatigue represents the most common side effect of radiation therapy. This is not ordinary tiredness; it is a profound exhaustion that a good night’s sleep does not cure. Your body uses massive amounts of energy to repair healthy tissue damaged by the radiation.
To manage fatigue, you must listen to your body. Rest when you feel tired, but also try to engage in light physical activity, like a 15-minute daily walk. Studies show that gentle exercise actually combats cancer-related fatigue better than total bed rest.
Skin Irritation
The skin in the treated area often reacts to the radiation. It may look red, feel sunburned, or become dry and itchy. In severe cases, it might blister and peel. Looking at skin reaction photos of radiation therapy can help you identify what constitutes a normal reaction versus an infection.
Manage skin changes by wearing loose, soft clothing made of cotton. Wash the area gently with warm water and mild, unscented soap. Do not scrub the skin or wash off your treatment marks. Ask your oncology team to recommend a specific, safe moisturizer, and apply it exactly as directed. Avoid using heating pads or ice packs on the treated skin.
Site-Specific Side Effects
Depending on where the radiation targets, you may experience other issues. Radiation to the head and neck can cause dry mouth, difficulty swallowing, or changes in taste. Radiation to the chest might cause a cough or shortness of breath. Abdominal radiation often triggers nausea or diarrhea. Your medical team will prescribe medications or recommend dietary changes to handle these localized side effects.
The Importance of Photos in Setting Expectations

We cannot overstate the psychological benefit of visual preparation. When you search for photos of radiation therapy, you strip away the mystery of the hospital environment.
Many treatment centers now offer virtual tours or photo galleries on their websites. Patients who review these resources report lower heart rates and less anxiety during their first few sessions. Seeing photos of radiation therapy masks, for instance, prepares you for the tight-fitting sensation. Seeing the laser lights used for positioning prevents you from feeling alarmed when the room goes dark.
By familiarizing yourself with photos of radiation therapy, you transition from a state of fear to a state of readiness. You become an active participant in your care rather than a passive recipient.
Expert Tips for a Smoother Experience
Navigating cancer treatment requires a proactive approach. Medical professionals recommend several strategies to improve your daily experience.
First, stay incredibly hydrated. Drinking plenty of water helps your body flush out toxins and aids in cellular repair. Aim for at least eight glasses of water a day unless your doctor advises otherwise.
Second, prioritize nutrition. Your body needs protein and calories to heal healthy tissue. If eating becomes difficult due to nausea or swallowing issues, switch to nutrient-dense smoothies, protein shakes, or small, frequent meals.
Third, ask questions. Write down your concerns between appointments and bring your list to your weekly doctor visits. Do not assume any question is too small or silly.
Fourth, seek emotional support. Cancer treatment takes a toll on your mental health. Join a support group, speak to an oncology social worker, or lean on family and friends. Connecting with others who understand the process provides immense relief.
Common Mistakes to Avoid
Patients often make minor missteps that complicate their treatment journey. Avoid these common pitfalls to ensure your therapy goes as smoothly as possible.
Using Unapproved Skin Products: Never apply random lotions, perfumes, or deodorants to the treated area without your doctor’s permission. Many commercial products contain alcohol or heavy fragrances that severely aggravate irradiated skin.
Ignoring Mental Health: Many patients focus entirely on their physical symptoms and ignore their emotional distress. Anxiety and depression can hinder your physical recovery. Address your mental health early.
Failing to Report Symptoms: Some patients try to “tough it out” and hide their pain or nausea from their doctor. This is a massive mistake. Your team can provide medications that drastically improve your quality of life, but they can only help if they know what you are experiencing.
Losing Weight Intentionally: Even if you carry extra weight, radiation therapy is not the time to diet. Weight loss changes the shape of your body. If your body shape changes significantly, your custom immobilization molds will no longer fit properly, and the radiation beams may miss their exact target.
Comparing External and Internal Radiation
Understanding the different delivery methods helps clarify your specific treatment plan. Here is a breakdown of the two main types of radiation therapy.
|
Feature |
External Beam Radiation |
Internal Radiation (Brachytherapy) |
|---|---|---|
|
Delivery Method |
A machine outside the body directs beams inward. |
Radioactive implants placed directly inside or near the tumor. |
|
Duration of Session |
10 to 30 minutes per daily session. |
Can remain in place for a few minutes, days, or permanently. |
|
Radioactivity |
You are not radioactive after the session ends. |
You may emit small amounts of radiation while the implant is active. |
|
Common Uses |
Breast, lung, prostate, head and neck cancers. |
Prostate, cervical, uterine, and eye cancers. |
|
Pain Level |
Painless during delivery; similar to an X-ray. |
Requires minor surgery or catheter placement; may cause localized discomfort. |
Deep Dive: The Science of Cellular Repair
To truly appreciate your body’s resilience during this process, it helps to understand the biology. Radiation therapy creates breaks in the DNA of all cells in its path. Healthy cells possess robust repair mechanisms. When radiation damages a healthy cell, its internal proteins immediately recognize the break and begin stitching the DNA back together.
Cancer cells, by their very nature, are defective. They prioritize rapid, uncontrolled growth over DNA maintenance. Therefore, when radiation shatters their DNA, they lack the organized machinery to repair themselves. They attempt to divide with broken DNA, which leads to immediate cell death.
This biological difference forms the foundation of modern radiotherapy. By delivering the treatment in small daily fractions rather than one massive dose, doctors give your healthy cells a 24-hour window to repair themselves while the cancer cells slowly die off.
How Family and Caregivers Can Help
Cancer affects the entire family, not just the patient. Caregivers play an essential role in the success of the cancer treatment plan.
Caregivers can assist by managing the logistics of daily appointments. Driving to the hospital every single day becomes exhausting for the patient. A reliable transportation schedule removes a massive burden.
Furthermore, caregivers should educate themselves by reviewing photos of radiation therapy and reading about the side effects. When a caregiver understands what the linear accelerator looks like and how the skin might react, they can provide grounded, calm support. They can also take notes during doctor visits, as patients often feel too overwhelmed to remember medical instructions.
The Role of Diet and Nutrition

What you put into your body significantly impacts how well you tolerate radiation therapy. Proper nutrition helps maintain your weight, preserves your strength, and rebuilds healthy tissues.
Focus on high-protein foods like lean meats, eggs, beans, and Greek yogurt. Protein acts as the building block for cellular repair. Additionally, incorporate healthy fats from avocados, nuts, and olive oil to keep your calorie count up if you lose your appetite.
If you receive radiation to your digestive tract or throat, you may need a specialized diet. Foods that are soft, bland, and easy to swallow become essential. Avoid spicy, acidic, or extremely hot foods that can irritate sensitive tissues. Your oncologist can refer you to an oncology dietitian who will tailor a meal plan exactly to your needs.
Looking Ahead: Life After Radiation
Completing your final radiation session brings a mix of relief and anxiety. You no longer have the safety net of daily medical supervision.
It is important to understand that side effects do not vanish the moment treatment ends. In fact, skin irritation and fatigue often peak a week or two after your final session because the radiation continues to work inside your body. It may take several weeks or even months for your energy levels to return to normal.
Your doctor will schedule a follow-up scan a few months after treatment concludes. The delay is necessary because the cancer cells take time to die and clear out of the body. Immediate scans often show inflammation that mimics cancer, causing unnecessary panic. Patience is crucial during this recovery phase.
Harnessing the Power of Visual Preparation
The overarching theme of a successful treatment journey involves eliminating the fear of the unknown. We highly recommend that you spend time viewing photos of radiation therapy before your simulation appointment.
Look at the sterile but highly advanced machinery. Look at the specialized tables. Look at the immobilization masks. Acknowledge that while the equipment looks intimidating, it represents the pinnacle of modern medical technology designed entirely to save your life.
When you pair this visual knowledge with the practical tips outlined in this guide, you transform yourself from a fearful patient into an empowered survivor. You understand the science, you know the daily routine, and you possess the tools to manage the side effects.
Conclusion
Understanding your treatment environment significantly reduces anxiety. Looking at photos of radiation therapy allows you to feel prepared for the journey ahead. Trust your medical team and communicate your needs openly throughout the process. Speak with your oncologist today to review specific images of the equipment they will use for your personalized care.
FAQs
1. What does a radiation therapy machine look like?
A linear accelerator is a large, white medical device with a flat treatment table. It features a massive gantry (arm) that rotates around the patient to deliver precise energy beams. Viewing photos of radiation therapy machines online can help you familiarize yourself with their intimidating size.
2. Does radiation therapy hurt?
No, the actual delivery of external beam radiation is completely painless. You will not feel, see, or smell the radiation. It feels exactly like having a standard X-ray taken.
3. Will I lose my hair during radiation therapy?
You will only lose hair in the exact area where the radiation beam enters your body. For example, if you receive radiation to your leg, you will not lose the hair on your head.
4. How long does a daily radiation session take?
You will spend about 15 to 30 minutes in the treatment room. Most of this time involves the therapist carefully positioning your body. The actual radiation delivery only lasts one to five minutes.
5. Why do they draw marks on my skin?
The radiation therapists use small ink marks or tiny tattoos to ensure they align the machine perfectly every single day. This guarantees the radiation hits the tumor precisely and spares healthy tissue.
6. What is a radiation mask used for?
If you receive radiation to your head or neck, the team creates a custom plastic mesh mask that fits snugly over your face and shoulders. It holds your head perfectly still so the radiation beams hit the exact intended targets.
7. Can I be around my family after external radiation?
Yes. External beam radiation does not make you radioactive. It is perfectly safe to hug your children, sleep next to your spouse, and interact with pets immediately after your session.
8. What are the most common side effects?
Fatigue and skin irritation in the treated area represent the most universal side effects. Other symptoms depend entirely on which part of your body receives the radiation.
9. Can I drive myself to my treatments?
Most patients can drive themselves to and from their daily sessions, especially during the first few weeks. However, if fatigue becomes severe later in the treatment plan, you may need a caregiver to drive you.
10. How soon will I know if the radiation worked?
Radiation continues killing cancer cells for weeks or months after your final session. Your oncologist will typically schedule follow-up imaging scans two to three months after treatment ends to accurately evaluate the results.