Facing a new medical diagnosis requires gathering the right information. Infusion cancer treatment remains one of the most effective and widely used methods to fight abnormal cells. This guide explains everything you need to know to approach your upcoming sessions with absolute confidence.
This comprehensive guide breaks down the mechanics of infusion cancer treatment, explaining how medications enter your bloodstream to target disease. You will learn about the primary benefits, explore practical ways to manage common side effects, and discover expert tips to make your therapy sessions more comfortable. We also cover critical mistakes to avoid and answer the most pressing questions patients ask.
What Is Infusion Cancer Treatment and How Does It Work?
Understanding the medical processes behind your care plan helps reduce anxiety and builds confidence. Infusion cancer treatment involves delivering powerful medications directly into your bloodstream through a needle or catheter. Unlike oral pills that must pass through your digestive system, this intravenous delivery method ensures that the drugs reach their target rapidly and at maximum potency.
Doctors use infusion cancer treatment to administer a wide variety of therapies. The specific liquid you receive depends entirely on your diagnosis, the stage of the disease, and your overall health profile. By placing the medication right into your veins, your cancer care team can tightly control the exact dosage and absorption rate. This precise control makes the therapy highly reliable for shrinking tumors, preventing the spread of abnormal cells, and alleviating severe symptoms.
The Mechanics of Intravenous Delivery
The delivery mechanism for infusion cancer treatment is straightforward but highly monitored. Nurses typically insert a small intravenous (IV) line into a vein in your arm or hand. For patients who need long-term care, doctors might surgically place a central line or a port under the skin of the chest. A port prevents the need for repeated needle sticks, making your weekly or monthly visits significantly more comfortable.
Once the line is secure, the medication flows from a sterile bag through a plastic tube and directly into your body. Depending on the prescribed drugs, a single session of infusion cancer treatment can last anywhere from thirty minutes to several hours. During this time, you sit in a comfortable chair while medical staff continuously monitor your vital signs.
Types of Medications Administered
Infusion cancer treatment is not limited to just one type of drug. Oncologists use this delivery method for several different pharmaceutical categories. Traditional chemotherapy is the most common, using cytotoxic drugs to destroy rapidly dividing cells. However, modern medicine has expanded the arsenal significantly.
You might receive immunotherapy through an IV, which stimulates your body’s natural defenses to recognize and attack foreign cells. Alternatively, targeted therapy focuses specifically on the genetic changes or proteins that allow tumors to grow. Many patients also receive supportive fluids, anti-nausea medications, and pain relievers through their IV to help manage the overall experience and maintain their strength.
The Major Benefits of Infusion Cancer Treatment
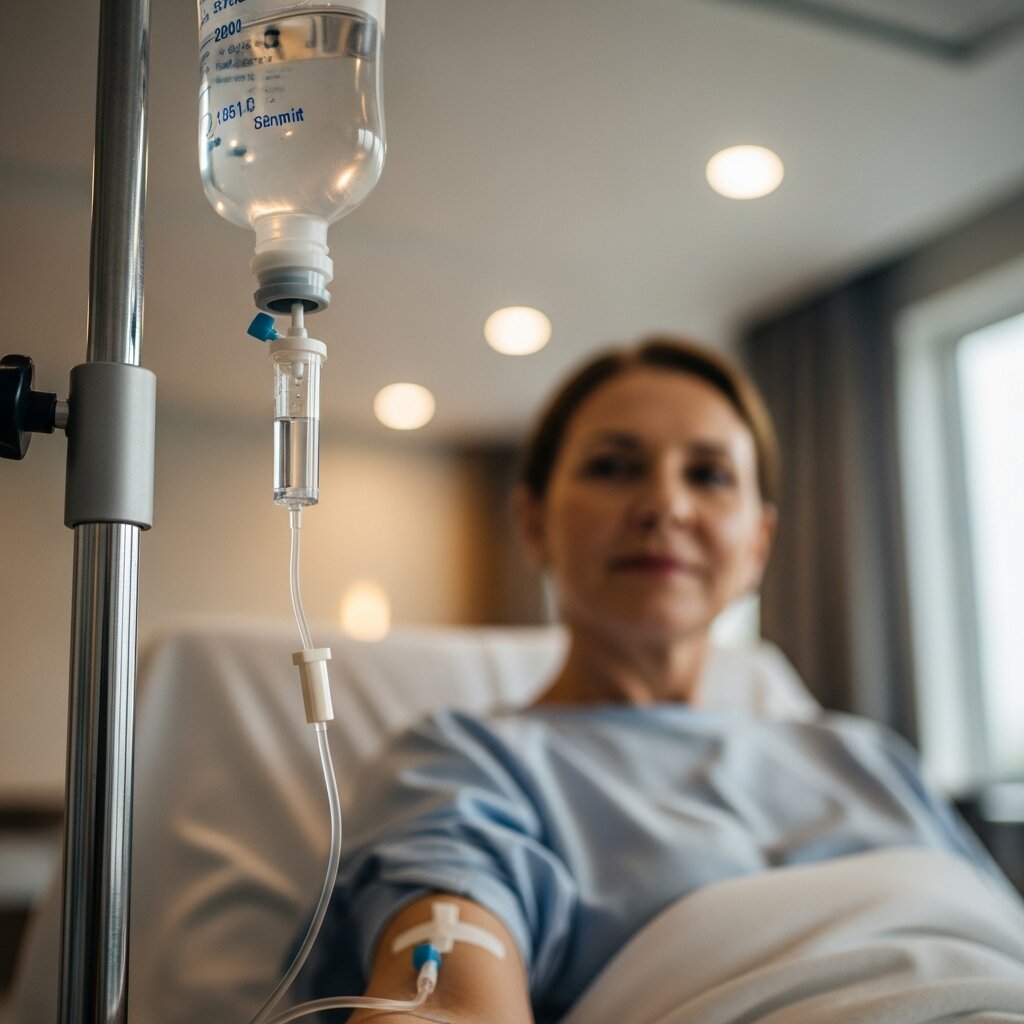
Choosing the right therapy path is a collaborative decision between you and your doctor. Infusion cancer treatment offers several unique advantages that make it a cornerstone of modern oncology. The direct-to-bloodstream approach provides clinical benefits that oral medications often cannot match.
One of the primary benefits of infusion cancer treatment is the immediate bioavailability of the medication. Because the drugs bypass the stomach and liver, they do not break down before reaching the affected tissues. This ensures that a highly concentrated, effective dose attacks the disease immediately.
Precision, Speed, and Medical Supervision
When you undergo infusion cancer treatment, your medical team controls the exact drip rate of the medication. If you experience an adverse reaction, the nurse can instantly stop the flow and administer counteracting drugs. This level of real-time supervision provides a safety net that at-home treatments lack.
Furthermore, infusion cancer treatment allows doctors to combine multiple therapies into one session. You might receive a targeted drug followed immediately by a supportive hydration fluid. This combination approach maximizes the therapeutic impact while minimizing the number of days you must spend in a clinical setting.
Bypassing Gastrointestinal Issues
Many patients struggle with digestion and nausea during their health journey. Taking strong oral medications can irritate the stomach lining, leading to vomiting and poor drug absorption. Infusion cancer treatment completely bypasses the gastrointestinal tract.
This means that even if you feel too nauseous to swallow a pill or keep food down, you can still receive your life-saving medication. The IV method guarantees that your body absorbs 100 percent of the prescribed dose, removing any guesswork from your recovery plan.
Comparing Infusion Cancer Treatment to Oral Therapies
|
Feature |
Infusion Cancer Treatment |
Oral Cancer Treatment |
|---|---|---|
|
Delivery Method |
Intravenous (IV), port, or central line |
Swallowed as a pill, capsule, or liquid |
|
Location |
Hospital or specialized clinical center |
Taken at home or anywhere |
|
Absorption Rate |
Immediate and 100% bioavailable |
Slower, depends on digestion |
|
Supervision |
Continuous monitoring by medical staff |
Self-administered by the patient |
|
Stomach Irritation |
Bypasses the stomach completely |
Can cause gastrointestinal distress |
Common Side Effects of Infusion Cancer and How to Manage Them

Because infusion cancer treatment uses powerful systemic drugs to fight disease, it inherently affects healthy cells alongside abnormal ones. This overlap causes the side effects most patients experience. Preparing for these physical changes helps you manage them effectively and maintain a higher quality of life.
The specific side effects of infusion cancer treatment vary wildly depending on the exact drugs used. However, some physical reactions are universally common. By working closely with your doctor and understanding your body’s signals, you can minimize discomfort.
Managing Physical Fatigue and Nausea
Fatigue is the most frequently reported side effect of infusion cancer treatment. This is a profound exhaustion that a simple nap cannot fix. Your body expends massive amounts of energy trying to heal and process the heavy medications. To manage this, you must prioritize rest and gently move your body only when you feel capable.
Nausea is another well-known hurdle. Fortunately, modern medicine offers incredible anti-nausea drugs that are often administered right alongside your primary infusion cancer treatment. You can also combat nausea by eating small, bland meals throughout the day rather than three large ones. Staying hydrated with clear fluids helps flush the toxins from your system faster.
Protecting Your Immune System
Many forms of infusion cancer treatment lower your white blood cell count, leaving you vulnerable to outside infections. This condition, known as neutropenia, requires strict hygiene practices. You must wash your hands frequently, avoid large crowds, and steer clear of anyone who is actively sick.
If you develop a fever during your therapy cycle, you must contact your doctor immediately. A fever serves as an early warning sign that your suppressed immune system is fighting an infection. Your medical team will likely monitor your blood counts before every single infusion cancer treatment to ensure your body is strong enough to handle the next dose.
Expert Insights: How to Prepare for Your First Session
Walking into a clinic for your first infusion cancer treatment feels intimidating. However, preparation completely shifts your mindset from anxious to empowered. Oncology nurses and long-term survivors recommend treating your infusion day like a scheduled long-haul flight.
Hydration plays a massive role in a successful infusion cancer treatment. Drink plenty of water the day before your appointment. Well-hydrated veins are plumper and much easier for the nursing staff to access, saving you from multiple needle pricks.
Pro Tips for Maximum Comfort
Dress in loose, comfortable layers. Clinical environments fluctuate in temperature, and you want easy access to your arms or chest port without feeling restricted. Bring a warm, familiar blanket from home to create a comforting environment.
Pack a dedicated bag for your infusion cancer treatment. Include a tablet with downloaded movies, noise-canceling headphones, and a good book. Time moves slowly in the infusion chair, so having multiple forms of entertainment distracts your mind. Finally, pack easy-to-digest snacks like crackers or ginger candies to settle your stomach during the drip.
Common Mistakes to Avoid During Treatment

Patients occasionally make errors that unintentionally complicate their infusion cancer treatment. By identifying these pitfalls early, you can keep your therapy timeline on track and protect your physical health.
One major mistake is suffering in silence. If you feel a strange burning sensation at the IV site, or if you suddenly feel short of breath, you must alert a nurse immediately. Never assume that pain during an infusion cancer treatment is normal. Immediate communication prevents severe allergic reactions and tissue damage.
Another frequent mistake involves using unapproved supplements. Many patients assume that over-the-counter vitamins are harmless. However, certain antioxidants and herbal supplements can severely interfere with the effectiveness of your infusion cancer treatment. Always hand a complete list of your daily supplements to your oncologist for approval before your first session.
Mini-Conclusion: Navigating the complexities of intravenous therapy requires patience, preparation, and open communication with your care team. By avoiding these common errors, you safeguard your healing process.
Conclusion
Infusion cancer treatment remains a highly effective, precise method for delivering life-saving medications directly into your body. By understanding the mechanics, maximizing the benefits, and utilizing expert strategies to handle side effects, you can approach your therapy with confidence and calm. Take charge of your health journey today by writing down your specific questions and scheduling a detailed discussion with your oncology team.
FAQs
1. What exactly is infusion cancer treatment?
Infusion cancer treatment is a medical procedure where powerful therapeutic drugs are delivered directly into your bloodstream through a needle or catheter. This method ensures maximum drug absorption and allows doctors to closely monitor your immediate reaction to the medication.
2. How long does a typical infusion session last?
The duration of an infusion cancer treatment varies significantly based on the specific medication. Some targeted therapies take only 30 minutes, while complex traditional chemotherapy regimens can take up to eight hours to safely administer.
3. Does the needle hurt during the entire infusion?
No. While you will feel a quick pinch when the nurse initially inserts the needle, the actual infusion cancer treatment is generally painless. If you experience burning, stinging, or swelling at the IV site during the drip, you should alert your nurse immediately.
4. Can I drive myself home after my appointment?
Doctors strongly advise bringing a family member or friend to drive you home after your first infusion cancer treatment. Many pre-medications, like anti-allergy drugs and anti-nausea medications, cause severe drowsiness and impair your ability to drive safely.
5. What should I wear to my infusion appointment?
Wear loose-fitting, comfortable clothing with layers. If you have a chest port, wear a V-neck or button-down shirt so the nurses can access it easily. Clinics are often cold, so bringing a sweater or soft blanket is highly recommended.
6. Will I lose my hair from infusion therapy?
Hair loss depends entirely on the specific drugs used in your infusion cancer treatment. While traditional chemotherapy often causes hair thinning or loss, many modern targeted therapies and immunotherapies do not affect your hair follicles at all.
7. Can I eat before and during my treatment?
Yes, you can usually eat before and during your infusion cancer treatment unless your doctor specifies otherwise. It is best to stick to light, bland foods like toast, crackers, or broth to prevent nausea while the medication enters your system.
8. How often will I need to receive infusions?
Your schedule depends on your specific diagnosis and the protocol designed by your oncologist. Some patients undergo infusion cancer treatment once a week, while others might go once every three or four weeks to allow their bodies to recover between doses.
9. What are the signs of an allergic reaction during treatment?
Signs of a reaction during infusion cancer treatment include sudden shortness of breath, a tight feeling in your chest, flushing of the face, hives, or extreme dizziness. Nurses monitor you closely to catch and reverse these symptoms immediately.
10. Can I still work while undergoing infusion therapy?
Many patients continue to work while receiving infusion cancer treatment, especially if they have flexible or remote jobs. You will need to learn how your body reacts to the medication first, as fatigue peaks a few days after the session, requiring you to adjust your work schedule accordingly.


